If you are experiencing any type of tooth pain or abnormality, you may be wondering do I need a root canal? Although root canals are restorative procedures that can save a tooth from falling out or being extracted, many people try to avoid the dentist if they think they need a root canal. Root canals become necessary procedures when decay-causing bacteria reach the innermost layer of the tooth. This causes an infection known as pulpitis that can continue to spread if the infection is not removed.
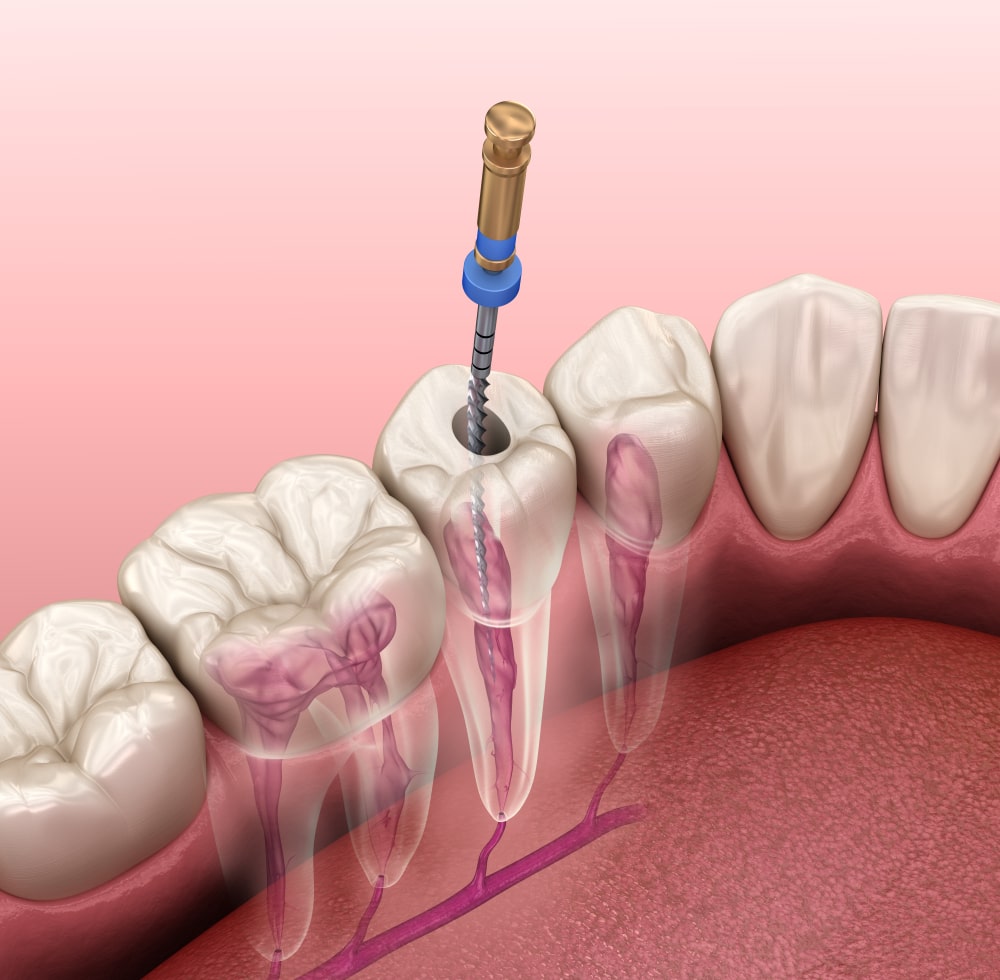
To preserve the tooth and to prevent the infection from spreading to the surrounding teeth, root canal therapy, also known as a root canal, is performed. During a root canal, a small hole is drilled in the tooth to reach the innermost pulp layer. The infected pulp tissue, blood vessels, and tooth nerve are then removed from the pulp chamber and root canals so that the inside of the tooth is completely empty. The empty tooth is then flushed with a microbial solution to prevent future infection before the tooth is restored with a dental crown.
While only your dentist can accurately diagnose a pulp infection and the need for a root canal, you may need a root canal if you are experiencing one or more of the following symptoms:
Tooth Pain
Tooth pain is a definite sign that something is wrong and it is one of the hardest symptoms to ignore. While tooth pain can have a variety of causes, tooth pain caused by pulpitis is described as being a deep, throbbing ache in the tooth and jaw. It is also said to come on suddenly and is known to get progressively worse as time goes on. There are cases where this pain comes and goes, as well as cases where the pain is constant. Pain associated with pulpitis also tends to get worse when chewing or when pressure is applied to the tooth. Finally, tooth pain caused by pulpitis can also take the form of tooth sensitivity. Tooth sensitivity is a sharp, sudden pain experienced in response to exposing the tooth to hot, cold, or sweet stimuli. Prolonged tooth sensitivity occurs when the painful sensation lasts even after the stimuli has been removed, and is another key sign of a pulp infection.
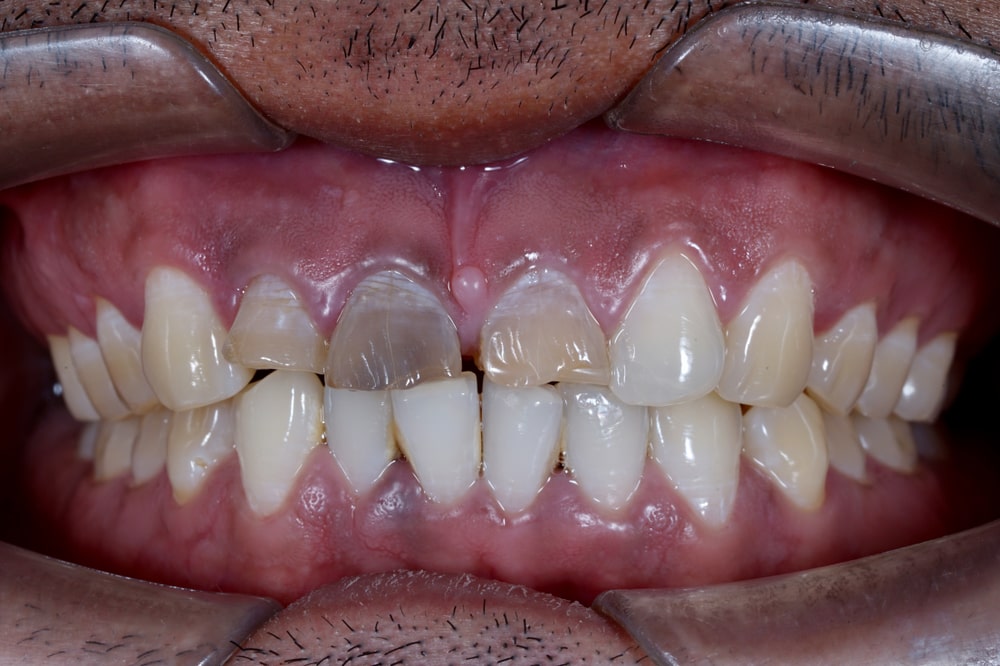
Discolored Tooth
Besides tooth pain, a pulp infection can also cause the affected tooth to become discolored so that it stands out from the other teeth. This can happen when the infection starts to kill off the pulp tissue inside the tooth. The result is a tooth that appears yellow, light brown, grey, or black. Even if you are not experiencing pain, a single discolored tooth should always be evaluated by your dentist.
Gum Problems
Despite the fact that pulpits primarily affect the inside of the tooth, it can also affect the gums. This is due to the fact that the bacteria responsible for pulpitis can also lead to gum disease. If you suddenly notice your gums becoming red, tender, or swollen, especially around the affected tooth, then this could indicate a pulp infection. In some cases, the gums around the tooth may also have pimples or discharge along the gum line. Just as pulpitis can spread to the other teeth, it can also cause gum disease to spread throughout the mouth.
The combination of sudden throbbing tooth pain, a discolored tooth, and gum problems can all indicate a possible pulp infection in need of a root canal. However, it is also important to notice that these symptoms can occur alone and still be associated with a pulp infection. These symptoms can also indicate another dental issue. In some cases, a pulp infection may not even cause symptoms and will only be identified through a dental x-ray. Since there is so much ambiguity associated with pulpitis symptoms, it is recommended to have your dentist perform an examination to determine whether pulpitis is present and if a root canal is necessary.